Plantar Fasciitis Treatment Los Angeles – Heel Pain Beverly Hills
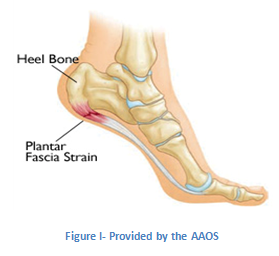
Plantar fasciitis is the most common cause of heel pain in the United States with over 2 million patients seeking treatment for this condition in the last year alone according to statistics published by the American Academy of Orthopaedic Surgeons (AAOS). Plantar fasciitis occurs when the plantar fascia, the strong band of tissue that supports the arch of your foot, becomes irritated and inflamed as shown in the image below provided by the AAOS. As a result of the inflammation your heel may hurt, feel hot, swell or turn red.

Plantar Fasciitis – Causes and Risk Factors
You’re more likely to get plantar fasciitis if:
- You are female
- You are overweight
- You have a job that requires a lot of walking or standing on hard surfaces
- You are a runner or participate in high activity sports
- You have tight calf muscles that limit how far you can flex your ankles
- You have very flat feet or very high arches
We Made Them All Happy
Kimberly D. / Los Angeles, CA
Plantar Fasciitis – Symptoms
Plantar fasciitis develops gradually with mild pain at the heel bone progressing to more severe pain as the injury gets worse without treatment. Although the pain may not interrupt your workout, you are very likely to feel it afterwards. The most common scenario described by sufferers of plantar fasciitis is severe heel pain that occurs right after getting up in the morning.
The most common symptoms of plantar fasciitis include:
- Pain on the bottom of the foot near the heel
- Pain with the first few steps after getting out of bed in the morning
- Pain after a long period of standing or sitting
- Pain that eases after a few minutes of walking
- Pain that is intense after (not during) exercise or activity
- Pain that affects just one foot (rarely it can occur in both feet at the same time)
- Pain that feels like you are being stabbed in the heel of your foot
Plantar Fasciitis – Diagnosis by Dr. Jamshidinia in Los Angeles
To make the diagnosis of plantar fasciitis, Dr. Jamshidinia will review your medical history and physically examine your foot. Imaging studies may also be useful to confirm the diagnosis of plantar fasciitis.
Medical History: Focusing mainly on your foot and heel, Dr. Jamshidinia will discuss all aspects related to the symptoms you are experiencing including:
- When it started
- Where it’s located
- What makes it worse
- What makes it better
- What activities you do
- Past Injuries
Physical Exam: Dr. Jamshidinia will check for points of tenderness in your foot. The location of your pain can help determine if it’s caused by other problems. A thorough physical exam may include testing your:
- Reflexes
- Muscle strength
- Muscle tone
- Senses of touch and sight
- Coordination
- Balance
Imaging Studies: Dr. Jamshidinia may use imaging studies to confirm the diagnosis, as well as get a better visual of the area to see if there are any other problems contributing to your symptoms.
- MRI- can show an impinged nerve or stress fracture
- XRay- can show a bone spur that is causing heel pain

Plantar Fasciitis Treatment at Tower Foot and Ankle in Los Angeles
If you don’t treat your plantar fasciitis, it can progress and become a chronic condition. You may not be able to keep up your current level of exercise and activity, and you may develop additional symptoms affecting your foot, knee, hip and back because chronic plantar fasciitis can change the way you walk. Treatment options for plantar fasciitis are broken down into 2 categories: non-surgical and surgical.

Non-Surgical Treatment for Plantar Fasciitis
Platelet Rich Plasma Therapy (PRP Treatment) – an increasingly popular and effective treatment option utilizing healing properties isolated from your own blood and injecting them into the plantar fascia to induce rapid healing response over 1-2 weeks. It has been made popular by top athletes who uses the treatment throughout the season and for major injuries such as his recent achilles tendon rupture.
One study showed that plantar fasciitis treated with platelet rich plasma therapy had longstanding healing effects on the plantar fascia compared to a control group that received methylprednisone steroid injection. PRP is done under local anesthetic with sedation if patient desires in a safe controlled environment in our surgical facility thus greatly reducing the minimal chance of infection.
Rest – Decreasing or even stopping the activities that make the pain worse is the first step in reducing the pain.
Ice – Rolling your foot over a cold water bottle or ice for 20 minutes is effective.
Nonsteroidal Anti-inflammatory (NSAIDS) – Drugs such as ibuprofen or naproxen reduce pain and inflammation.
Physical therapy – Stretching your calves and plantar fascia is the most effective way to relieve the pain that comes with this condition.
Cortisone Steroid Injections – A powerful anti-inflammatory medication can be injected into the plantar fascia to reduce inflammation and pain.
Custom orthotics – Custom shoe inserts will provide extra cushioning to reduce tension while standing and walking.
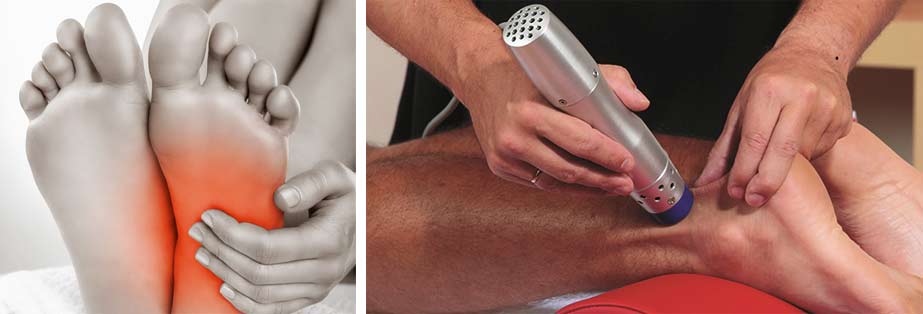
Extracorporeal Shockwave Therapy (ESWT) – High-energy shockwave impulses stimulate the healing process in damaged plantar fascia tissue. ESWT is noninvasive procedure with minimal risks, offering an excellent alternative to surgery.
Surgical Treatment for Plantar Fasciitis
Plantar Fascia Release – In this procedure the plantar fascia ligament is partially cut to relieve tension in the tissue. If you have a large bone spur, it will be removed, as well.
Gastrocnemius Recession – A rare treatment option where the calf muscle (gastrocnemius) is surgically lengthened to relieve stress on the plantar fascia.

Plantar Fascia Stretching Exercises
The American Orthopaedic Foot & Ankle Society (AOFAS) has published specific exercises for the plantar fascia:
- Cross your affected leg over your other leg.
- Using the hand on your affected side, take hold of your affected foot and pull your toes back towards shin. This creates tension/stretch in the arch of the foot/plantar fascia.
- Check for the appropriate stretch position by gently rubbing the thumb of your unaffected side left to right over the arch of the affected foot. The plantar fascia should feel firm, like a guitar string.
- Hold the stretch for a count of 10. A set is 10 repetitions.