Having diabetes already proves a significant challenge in many patients’ lives. There are numerous symptoms to address and plenty of lifestyle restrictions. One severe and most times completely painless result of diabetes can be a diabetic foot ulcer. These are non-painful open sores or wounds and can significantly decrease your quality of life until they are treated. When left untreated, diabetic foot ulcers can lead to:
- Bone infections
- Limb threatening foot infections
- Cellulitis
- And even gangrene
Table of Contents
Toggle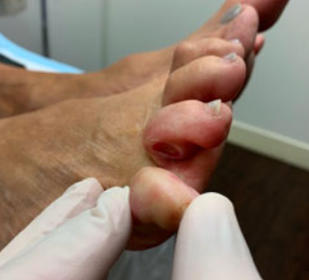
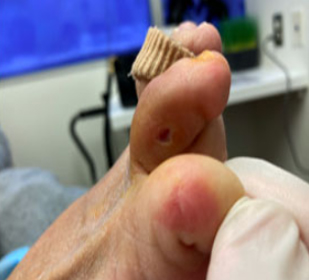
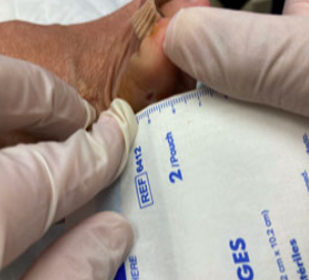
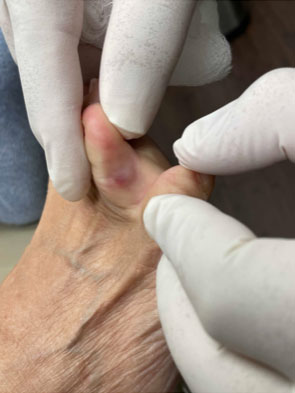
83 yo female with well controlled Diabetes-
Here presenting to our wound center for higher level of care to treat chronic non healing neuropathic diabetic foot ulceration. This patient received advanced topical medications, bioburden management and off loading to achieve progressive healing over very short period of time without hospitalization or surgery.

What Is a Diabetic Foot Ulcer?
Diabetic foot ulcers are a result of skin tissue breaking down and beginning to expose the lower layers. Typically, they appear in diabetic patients who might have not properly controlled their condition. Constantly treating and addressing diabetes can be challenging, and even a small slipup might be enough to allow an ulcer to develop.
Most often, they form either on your big toes or the balls of the feet. If left untreated, they progressively worse until they can affect the bones beneath the skin. That is why we recommend receiving treatment as soon as you feel one beginning to develop! The sooner you treat a diabetic foot ulcer, the easier it will be.
What is a Foot Wound?
Symptoms of Diabetic Foot
Diabetes can cause severe, even life-threatening complications to your feet. As mentioned above, the increased accumulation of blood sugar caused by diabetes causes downstream effects to your nerves and blood vessels. There are several symptoms that this causes in your feet including:
- Decreased blood flow to the feet
- Decreased healing ability in the feet
- Tingling and/or numbness of the feet
- Decreased ability to fight off infections in the feet
- Loss of sensation in the feet
- Loss of pulses in the feet
What Is So Dangerous About a Diabetic Foot Ulcer?
The root cause of diabetic foot ulceration is a lack of protective sensation to the feet. In medicine, when diabetic patients have no foot sensation (i.e., their feet are numb, feel tingly most of the time, or burn), we call this diabetic neuropathy. This term simply means nerve damage to the nerves of the feet.
Diabetic nerve damage or diabetic neuropathy can cause a patient to walk on something sharp or hot and not feel it. Likewise, they might walk with a tight-fitting shoe and not feel how tight it is. This can quickly lead to skin breakdown and infection, even within a few minutes.
We always remind our diabetic patients of a patient of ours who left a metal shoehorn in his shoe and went to work. Although this example sounds unfathomable, such things happen frequently. Other patients have pebbles inside their shoes, or a sock bunched up and causing irritation. Before they know it, they have developed a diabetic foot ulcer.
As a diabetic, be very mindful that temperature sensation may be abnormal and lead to your feet becoming burned from excessively hot water or walking on hot sand at the beach.
Complications of Diabetic Foot
- A loss of feeling in your feet.
- Foot ulcers or sores that do not heal.
- Dry Cracks in the Skin.
- Ingrown Nails or Fungal Nails.
- Swelling.
- Corns and calluses.
- Amputation.
Where Do Diabetic Foot Ulcers Form?
- Your big toes
- The balls of the feet
- On top of hammertoes
- Under a skin callus
- Areas associated with bony prominences like over bunions
Skin calluses are usually the site of future diabetic foot ulcers. A diabetic patient should approach these spots as a “warning sign” and get regular treatment by our office to prevent the callus from breaking down in the future. These are hot spots or pressure points that are most vulnerable to ulceration.
What Happens if a Foot Ulcer Is Not Treated?
- Become infected
- Lead to a limb-threatening or foot threatening infection
- Cause bone infection (osteomyelitis)
- A dark callus
- A callus that is thick or uncomfortable
- Bleeding
Remember, pain is not going to alert you, given diabetic neuropathy masks pain. Thus you can walk for many days with a vulnerable wound without knowledge of its presence.
You will not feel one beginning to develop, so make sure you routinely check your feet and have regular foot care by our office to prevent problems. The sooner you identify a diabetic foot ulcer or ulceration and get treatment, the more likely you can prevent amputation or infection.
What Are My Diabetic Foot Ulcer Treatment Options?
Treating a foot ulcer takes two forms: prevention and restoration.
When you visit Dr. Jamfeet, we will work with you to develop a personalized treatment plan. Each treatment focuses on addressing your unique concerns, including:
- Location of the ulcer
- Your current health
- Whether the ulcer is infected
Hyperbaric Oxygen Therapy for Foot Ulceration (HBO Therapy)

Foot Protection
- Diabetic Shoes
- Casts
- Compression Wraps
- Foot Braces
- Custom Shoe Inserts
Infection Prevention
If you have a diabetic foot ulcer, it is vital to prevent infection. Once infected, they become much more serious and more challenging to treat. This is why it is crucial to seek treatment as soon as you think you might have an ulcer.
Ways we might help prevent infection from occuring include:
- Skin disinfection
- Dressing it with anti-bacterial wraps
- Foot baths
- Enzyme treatments
Treating Infected Tissue
If an ulcer has progressed to a dangerous point, it must be treated right away.
Medication: In some cases, antibiotics may be enough to deal with an infected ulcer. We will take a sample of the infected tissue to determine if this treatment is best. Other medications include antiplatelets and anti-clotting drugs.
Debridement: This treatment removes the dead skin, foreign material, and infections that may have been the ulcer’s initial cause.
Surgery: Though usually not necessary, sometimes surgical methods can relieve pressure around the ulcer. Sometimes infections will require emergency surgery or even amputation and IV antibiotics along with prolonged hospitalization due to foot ulceration.
Fat Pad Augmentation: Some calluses are due to direct pressure from boney prominences in areas of the foot where the natural protective fat pad has been lost. Replacement of the fat pad can be performed to help restore cushioning to reduce pressure and potential for ulceration.
How Do I Know I Have a Diabetic Foot Ulcer?
During the early stages, patients might not feel any pain. So, it can be difficult for many to spot the symptoms. Below are some signs to watch out for. If you notice you have any of these, call us immediately to receive treatment!
Cracked Dark
This is the number one indication that ulceration has begun. If you see a cracked dark callus, seek treatment immediately to prevent it from worsening.
Drainage
One of the earliest signs is drainage from your foot. You might notice leakage in your socks or shoes, or some stains in your socks. Other signs of drainage are odors coming from the affected foot.
Inflammation
You may also notice swelling, redness, or irritation in the affected foot. These usually start out quite mild but quickly develop into constant noticeable discomfort.
Black Tissue
This is a visible sign of a foot ulcer that has become quite serious. If you see any blackened tissue on your foot around the ulcer, we advise immediate treatment from a specialist. It could be the beginnings of gangrene, which could result in severe complications.
Factors That Increase Your Risk
Though any patient with diabetes is at risk for developing foot ulcers, some factors increase your chances of them. Fortunately, many of these are simple lifestyle choices that you can easily change to protect yourself. Some, like quitting smoking, may be a challenge. But it is well worth it in the end.
Risk factors include:
- Poorly-fitted shoes
- Insufficient hygiene
- Higher levels of alcohol or tobacco usage
- Heart or kidney disease
- Obesity
- Eye disease from diabetes
- Improper trimming of toenails or calluses by a non-professional
- Poorly controlled Diabetes
- Diabetic Neuropathy
The Podiatrist’s Role in Diabetic Foot
- Diabetics with no risk -> yearly foot examinations are fine.
- Diabetics with some risk factors -> twice a year screenings at a minimum
- Diabetics with existing foot problems (ulcers, corns, etc…) -> should be seen frequently
- Diabetics with new acute symptoms or problems -> should be seen immediately.
Patients with diabetes that have lost sensation in their feet due to peripheral neuropathy and no longer feel pain in their feet are at the greatest risk for experiencing severe complications. These patients must be extremely cautious and inspect their feet everyday with the help of a family member or caretaker if they are unable to do so themselves to look for any areas of injury, irritation, cuts or sores.
Schedule Your Consultation
Timing is crucial when dealing with a diabetic foot ulcer. The longer you wait, the more you put yourself at risk. If you think you have a diabetic foot ulcer, call us today to schedule a consultation. Dr. Jam and his team will examine your foot and work with you to develop a treatment plan. Living with diabetes can be enough of a challenge, so don’t let a foot ulcer impact your life as well. During your consultation, Dr. Jam and his team will also provide key tips on how to prevent future ulcers from forming.